Faculty Focus
Norman Yanofsky, M.D.: Ready for any emergency
By Laura Stephenson Carter
In the 1960s, when Norm Yanofsky was just a kid, hospitals didn't have emergency departments. Even those with designated "emergency rooms" were likely to staff them only with residents or junior physicians. During the 1970s, as Yanofsky was progressing through college and medical school on his way to becoming a doctor, emergency medicine was on its way to becoming a specialty. Then, in 1977, when he was a fourth-year medical student at Tufts, Yanofsky took an elective in emergency medicine at Cardinal Cushing Hospital in Brockton, Mass. "I thought it would be good preparation for family practice," he says. But he fell in love—with emergency medicine. "I liked the variety. I liked the action. I liked the pace."
|
|
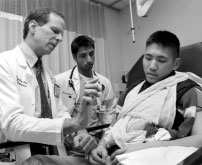
Yanofsky sees patients (above, left), oversees the administration of the Emergency Department at DHMC, and teaches residents and medical students as well as EMTs and ambulance squads all over the state (facing page). |
That same year, Yanofsky applied to five out of the 10 emergency medicine residency programs then existing in the U.S. and ended up at Northwestern. In 1979, emergency medicine was officially recognized as a specialty. And in February of 1980, more than 600 emergency physicians sat for the specialty's first certification exam. Yanofsky took the exam soon after, and has been board-certified in emergency medicine since 1982.
Today, the boy who literally grew up during the years when his chosen field was maturing is the medical director of the Emergency Department (ED) at DHMC. And while DHMC is not among the 140 institutions that today offer an emergency medicine residency—an institution's ED must see at least 35,000 patients a year to be eligible, and DHMC sees only about 21,000—the post has presented plenty of opportunities for someone who thrives on challenge and change.
It wasn't long after he completed his residency in emergency medicine and internal medicine, in 1981, that Yanofsky had a chance to return to the Northeast. First, however, he put in another year in Chicago—as a staff emergency physician at St. James Hospital and as an attending in emergency services at Northwestern Memorial Hospital —but he was ready to make a move either to Boston, where he'd grown up, or to the Upper Valley, where he had spent vacations and weekends hiking and skiing. So when a position opened up at DHMC in 1982, he grabbed it.
"When I came, I was the only staff physician in the emergency department," he says. "Things were very different then. The residents saw all the patients and my job was to provide quality assurance and teaching, to develop teaching programs across the region, to become involved in local and regional emergency medical services activities . . . [and] be part of the state oversight of emergency medical services."
He oversaw the residents assigned to the ED—one medical resident, one surgery resident, and an intern—as well as the emergency room nurses. At that time, medical residents generally did a month's rotation during each year of their residency, and surgical residents did a month during their second year. The department grew slowly, with another part-time physician hired the second year and a third the next. "We were directly involved if there was a dif- ficult patient or if it just got so busy that the resident was overwhelmed," Yanofsky explains. "But for the most part, we weren't staffing the emergency department per se."
Yanofsky also had administrative and teaching responsibilities—for medical students as well as residents—and he taught emergency medicine to healthcare providers throughout New Hampshire. "We ran four regional statewide conferences a year to teach people emergency medicine," he says. "I [also] would go around to EMS and ambulance squads and other hospitals to teach the local squads in that region."
Back then, the emergency room wasn't nearly as busy as it is today; in the early 1980s, only about 13,000 patients a year came through, Yanofsky recalls. "At that time, we saw a fair number of walk-ins," he says. And only about 9,000 of those 13,000 patients would be considered sick enough to be seen in an emergency room by today's standards. "I'd say, at that time, we saw a higher percentage of minor injuries, minor illness, which are much easier to take care of. Of course, we always saw patients with chest pain, belly pain, and the like, but the proportion of those patients has gone up. . . . Patients—elderly patients, with complicated medical histories, on eight to ten medications at a time—come in with complicated problems—sepsis, chest pain, breathing problems, neurologic problems—that take a lot more time to sort through."
Today, EDs everywhere are being bombarded with patients, and DHMC is no exception. Yanofsky attributes the increase to the growth and aging of the population in the region. In addition, DHMC added an air ambulance service in 1994, became a designated Level I Trauma Center in 1996, established a mobile intensive care unit (MICU) in 2000, and is now in the process of expanding its ED facilities to accommodate the increase in patients.
Yanofsky played a critical role in getting the Dartmouth-Hitch- cock Air Response Team (DHART) helicopter service up and flying. "That's one of the major accomplishments we've been able to pull off," he says proudly. In fact, although DHART didn't get off the ground until 1994, Yanofsky and others were exploring the idea of starting an air rescue service back in the early 1980s. "There was a head nurse, Susan MacKenzie, who had been in Vietnam. She got used to working with air transport—with helicopter transport of injured patients—and obviously saw it firsthand, saw how it worked and the benefits it provided." But there was no space for a helicopter to land at the Medical Center when it was located in Hanover, and, in addition, DHMC was not yet a designated trauma center and thus didn't have the capacity to handle the kind of seriously ill and injured patients that a helicopter would likely bring in.
"The problem is we have lots of little hospitals in New Hampshire and Vermont that are anywhere from 30 to 100 miles away and that rely on us . . . to take care of all their seriously injured or ill patients," explains Yanofsky. "It's hard for them to get those patients to us. It's a long drive in many cases. They often need critical-care personnel on the ambulance who aren't available immediately in these local hospitals. We saw all of that," he says, "and we knew that helicopters travel fairly quickly and they travel in a straight line and they really cut the transport time considerably."
I'll never forget the first day," Yanofsky says of DHART's inauguration. His eyes light up as he tells the story. "That was just a great day. We had no idea what was going to happen. I thought it might be two weeks before anybody called us. We went on-line at 7:00 in the morning on July 1, and within 15 minutes we got called down to Springfield, Vt. It was a scene call—an unconscious patient in an automobile accident. I think we had seven calls that first day, and we did six of them. In fact, one of our crew members was so tired and got so dehydrated they had to give her IV-fluids just to keep her going."
Most recently, Yanofsky had a hand in developing a sort of ground version of DHART—the mobile intensive care unit, or MICU. As with DHART, DHMC provides the medical staff, making it unnecessary for the hospitals involved in sending or receiving patients to provide the critical-care teams needed to monitor seriously ill or injured patients during transport. "Programs that have started with air transport have expanded to ground," says Yanofsky. "That's becoming more common around the country. A lot of times you can't go by air or the patient's not sick enough to require air transport."
When Yanofsky was hired by DHMC, he was also asked to play a key role in statewide emergency systems activities—something he still does. He was president of the New Hampshire chapter of the American College of Emergency Physicians from 1984 to 1986, and he chaired the New Hampshire Medical Society's Section of Emergency Medical Services from 1983 to 1985.

|
|
Today, EDs everywhere are being bombarded with patients, and DHMC is no exception. |
He also played a key role in developing a long-range plan for statewide emergency medical services in the 1980s. Some of the things in that plan that have now come to pass include enhanced 911 service, provision of automatic defibrillators in all ambulances, and a requirement that all ambulance staff be certi- fied at the EMT level or higher.
Yanofsky is also the longest-serving member of the EMS Trauma and Coordinating Board, a statewide group that oversees policy, approves rules and regulations, and helps to write legislation. And he was a founding member of an organization now called the EMS Medical Control Board, which, he says, "has turned into a very important group." It develops medical policy and creates all the state's protocols for paramedics and prehospital personnel.
Today, DHMC's ED is a very different place than it was when Yanofsky joined the faculty. It's much busier, and although residents are still an integral part of the team, there are now 10 staff physicians —five of whom are full-time.
"It is a national expectation that the majority of patients be seen by an attending," Yanofsky explains. Typically, "the resident will see a patient first, then present the patient to us, and then we'll see the patient." Or, in some cases, he says, "We'll see the patient directly."
After hours, Yanofsky plays keyboard and sings with a band called Y.B. Reasonable, which performs at DHMC functions such as office parties, as well as at other public events. "We play rock and roll and blues and jazz," he says. "I was in a band in high school and college for a few years. Then I stopped, from about third year of medical school, when things started getting intense." But he picked up music again about eight years ago. He also enjoys fishing with his 13-yearold son and watching his 11-year-old son play hockey.
But as much as anything, Yanofsky loves emergency medicine; he's still as passionate about the field as when he took that elective in medical school. "It's a wonderful specialty," he says. "There are a wide variety of things you can do—you can go anywhere in the country, you can be in a small community hospital, a rural hospital. You can be in a busy city emergency department, seeing gunshot wounds and violent trauma. You can be in an academic medical center and be doing research. You can work part-time and pursue other interests—it lends itself to that as well. You're not confined to a full-time career, if that's what you choose.
"You never know what your day is going to be like," he continues. "There are always challenges. But the downsides are you're going to work nights and weekends through your whole career on a routine basis. There are some patients who are not friendly and not easy to deal with, sometimes violent, hostile. And sometimes the working conditions get out of control."
But "we deal with that pretty well here," he concludes. "The patients here are . . . just nice people."
Laura Carter is the associate editor of Dartmouth Medicine magazine.
Both Photographs are by Jon Gilbert Fox.
