"Plastic firefly" gets a close look at the intestine
What is smaller than a quarter, weighs just four grams, and can be swallowed easily with a sip of water? The M2A diagnostic capsule, an ingestible "camera pill" that DHMC gastroenterologists Peter Anderson, M.D., and Steven Bensen, M.D., have found invaluable in hunting down obscure bleeding sources, gastrointestinal (GI) ulcers, and tumors in the twisted passageways of the small intestine.
DHMC was one of the earlier places in the country to use the new technology. Anderson and Bensen have now used the M2A on over 70 patients.
|

|
| |
|
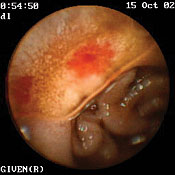
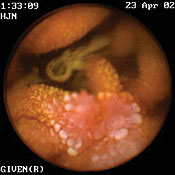
At right, Dartmouth gastroenterologist Peter Anderson shows off the M2A capsule
that helps doctors locate problems in the intestine. At left are a pair of M2A images:
an arteriovenous malformation (top) and a Crohn's disease lesion (bottom). | |
Methods: Conventional methods of examining the small intestine (including x-ray, enteroscopy, and colonoscopy) fail to detect disorders in 5% of patients with obscure GI bleeding. Barium x-rays pick up less than 10% of bleeding sources; arteriographies (x-rays involving a catheter) work only in cases of severe, steady bleeding; and push enteroscopies (the insertion of a GI endoscope from above) can only probe the first 5 to 10 feet of the 20-foot small intestine. All other patients have required intraoperative enteroscopy.
Using the new M2A capsule has proven both less invasive and much more effective. After an early European trial, researchers reported that push enteroscopy had identified a bleeding source in 9 of 32 patients, while the M2A procedure was successful in 21 of 32 patients.
The capsule consists of a lens, two tiny LED light sources, a camera on a computer chip, and a low-power radio transmitter. It is powered by two silver oxide batteries and is wrapped in a watertight casing.
Sensors: After the patient swallows the capsule, it moves through the digestive system, blinking all the way like a plastic firefly and transmitting video signals— two images a second—to sensors on the patient's abdomen. The sensors send signals to a wireless receiver that the patient wears on a belt. Six to eight hours later, the capsule passes through the body naturally and the equipment is removed.
Some 55,000 images are then downloaded from the receiver into a computer program that displays each image in sequence, so that doctors can see the entire small intestine, inch by inch.
The M2A is most useful in locating arteriovenous malformations— tangles of blood vessels on the surface of the small bowel's lining. Anderson says it can also find "early Crohn's disease, a common inflammatory bowel disease that sometimes can be very difficult to pick up on all the other techniques." In addition, it can detect early signs of cancer and small-bowel ulcers.
"The drawback of capsule endoscopy is that at this point it's only diagnostic," says Anderson. "It can see abnormalities, but it can't do anything about them," so some cases still require intraoperative enteroscopy. But the M2A "increases our chances of finding the culprit."
Anderson and Bensen are now planning a study to see if the M2A can help in identifying small-bowel causes of chronic abdominal pain.
Matthew C. Wiencke
If you would like to offer any feedback about this article, we would welcome getting your comments at DartMed@Dartmouth.edu.
