Faculty Focus
Daniel Levin: Saving little lives
By Laura Stephenson Carter
A concerned and tired-looking father, whose 19-month-old son has been diagnosed with meningitis, listens quietly while a pediatric resident reads aloud from the boy's medical chart. They're standing just outside the child's room in DHMC's Pediatric Intensive Care Unit (PICU), along with a social worker, a nurse, and the PICU's medical director, Daniel Levin, M.D. Occasionally, Levin (pronounced "luh-VIN") interrupts to define a technical term or to reassure the father that the infection was picked up promptly. "This could have been a lot worse," Levin tells him. After more discussion, Levin and the resident put on masks and enter the room to examine the little boy.
It's a typical morning in the PICU, where physicians, nurses, respiratory therapists, social workers, medical students, and parents are all routinely included on rounds. Levin says that everyone makes an effort to discuss medical information in plain English when family members are present. And parents aren't afraid to ask questions. He wishes he had included parents on rounds long ago, when he first started his career in pediatric intensive care medicine.
|
|
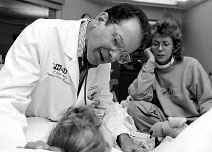
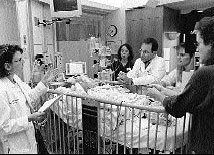
Even as he's tending to the needs of his young patients in Dartmouth's
pediatric intensive care unit (above), Dan Levin is
also conferring with parents and the nurses, residents, medical
students, and other caregivers in the unit (facing page). |
Levin, who is considered a pioneer in the field, was a medical student at the University of Illinois in Chicago when his rotations first sparked an interest in pediatric critical care. "When I was a junior medical student in 1967, we rotated through several hospitals— University of Illinois, Cook County, Rush Presbyterian, St. Luke's. In all those hospitals, right from the very beginning, I noticed that the pediatric patients were very sick and would be on the ward in regular rooms with no specialized care," he says. "At that very early stage, I was forming the idea that there needed to be more organized medical care for very sick pediatric patients."
He was soon making a difference. When Levin began his pediatric residency at St. Luke's Hospital in 1969, he was instrumental in opening a four-bed PICU there. After completing his residency in 1971, he did a cardiology fellowship at Children's Memorial Hospital in Chicago, which already had a PICU. But there, he observed a lack of coordination in the care of patients on the unit. "The physicians taking care of patients were either medical people or surgical people, coming in and out taking care of their individual patients," he says. "Nobody overall was taking care of them, except for the anesthesiologists —they were the only ones who knew how to ventilate children."
So Levin's next step was to do a perinatology fellowship at the Cardiovascular Research Institute of the University of California at San Francisco. In the early 1970s, pediatric anesthesiologists brought to PICUs "their particular knowledge and skills from anesthesia," says Levin. "So I thought I would bring circulatory and respiratory physiology skills, by taking cardiology and neonatology—never intending to be a cardiologist or a neonatologist—and say I was a pediatric intensivist."
In 1975, after finishing the two fellowships, Levin was recruited to Children's Medical Center in Dallas to start a pediatric intensive care unit with anesthesiologist Frances Morriss, M.D. Pediatrician-run units were rare at the time. "People like me were first starting to develop full-time pediatric intensive care unit services [run] by pediatricians," says Levin.
But pediatric critical care medicine wasn't yet recognized as a specialty. In May 1979, at a meeting of the Society for Critical Care Medicine, Levin and a dozen others met to discuss pediatric critical care issues. The group petitioned the society to create a pediatric section. "Now the section has 1,000 members," Levin says. But it still wasn't until 1987—when the first certifying exams in pediatric critical care were given—that physicians could be boardcertified in the specialty.
Also back in 1979, Levin coauthored one of the first textbooks on pediatric intensive care. "Fran Morriss and I had a sense that we were saying the same things over and over and over again on rounds and at teaching conferences. We decided to write them down so people could read about them," Levin says. "That led to a small book on pediatric intensive care, which was probably one of the first books out there. Nurses, students, residents, respiratory therapists, and other physicians were very hungry for this type of information.
There were a lot copies sold in the United States," Levin says of the book, and "it was translated into several languages. Fran and I would get Christmas cards from people in India and in Taiwan and places like that, saying that they felt like they knew us because they used our book every day."
And at a recent conference, Levin adds, he met a respected senior pediatric intensivist who told him an amusing story. "He said that when he was a resident, there was just one attending in the intensive care unit," Levin says. "When the fellow had to be out of town, he would give [the residents] our book and say, 'Just do what it says in here and you'll be okay.'"
That book—A Practical Guide to Pediatric Intensive Care, now renamed Essentials of Pediatric Intensive Care—is in its fourth edition and is still being used worldwide. "The irony of it is that people all over the world were using it and reading it, but Fran and I had to keep saying the same things over and over again on rounds, because our own people didn't use it," Levin says with a laugh. "I guess they felt we were right there and they didn't have to read it. They could just get it from us verbally."
While Levin was busy caring for critically ill children, as well as overseeing the administrative aspects of the PICU, some parents enlisted his help in trying to prevent a problem that had reached enormous proportions—drownings and near-drownings of young children. "It was a huge, epidemic problem in the South, particularly in Texas and a place like Dallas," Levin says. "In the states of California, Arizona, Texas, and Florida, it was the leading cause of death, after the newborn period, in small children. We would get 20, 30, 40 patients in the summer in the intensive care unit." Other area hospitals saw many drowning victims, too.
|
|
Levin, who is considered a pioneer in the field, wishes he had included parents on rounds long ago. |
"We went first with a state-wide agenda to Austin to try and get pool safety legislation passed," says Levin, who from 1984 to 1995 headed an organization called Seeking Positive Leadership Against Swimming Hazards (SPLASH). "We met with defeat. The representatives and state senators from west Texas, where they would get two drops of rain in the entire year and there were no swimming pools, didn't want to have anything to do with it. We eventually did get an ordinance passed in Dallas . . . for safety fencing."
But although fencing kept neighbor children away from pools, it did nothing to save children who actually lived in homes with pools. "What they would do is toddle out of their own house into the backyard and drown in the pool," says Levin. "Or their parents would put them in the backyard to play in January on a nice 50-, 55-degree, sunny day, and there'd be no fencing between the child's sandbox and the pool. They'd find the child fully clothed on their tricycle in the pool."
Levin was surprised at how difficult it was to get the life-saving legislation passed. "It was hard, it was really hard," he says. "It's so obvious to you that it's important, and nobody else cares. We fought stiff resistance from the pool industry, from fence builders, because they were worried that they would be held liable if their fence failed. They cared more about the liability than they cared about the children, about trying to do the right thing." There was also opposition from contractors and real estate agents, who "were afraid they couldn't sell a house if it didn't have everything in place." He shakes his head and says softly, "It was pretty depressing."
Another focus for Levin has been exploring how to help parents understand the meaning of brain death. The concept of brain death can be very confusing, he says. "Some of it is the language used. It makes sense that society, the law, medicine, religion all need a way of saying somebody's dead, even though they're on these machines. But then they turn around to families and say, 'We're going to withdraw the life support systems now.' Well, they're not life support systems," Levin says. "The patient's dead. The terminology is inherently confusing to families."
So now, he explains, "we talk about going from diagnosing the patient as brain dead, pronouncing the patient dead, and then talking directly to the family about arranging for funerals, religious services. We focus them on the natural progression of life events and death events and turn their focus away from the equipment."
Until 1996, Levin was the medical director of the PICU at Dallas Children's Medical Center, as well as of the pediatric trauma intensive care unit at Dallas's Parkland Memorial Hospital. The two units had grown from 10 to 38 beds in the time he was there, and there were plans for further expansion to 50 beds. And, by the time he left, he and Morriss had trained more than 55 fellows from all over the world. On top of that, Levin's resume listed over 120 lectures; more than 100 papers, abstracts, and book chapters; several books; and leadership roles on countless state and national committees and boards.
But doing all that as well as practicing pediatric intensive care medicine in a fast-paced, urban environment for over 20 years was "very frantic and very physically and psychologically taxing," Levin explains. "There weren't many people who had started at the time I had who were still practicing pediatric intensive care at that pace." Levin was ready to move on.
At a propitious moment, a longtime friend—someone Levin had trained with in San Francisco in the early '70s—called. John Brooks, M.D., then chair of pediatrics at Dartmouth, told Levin that DHMC was looking for a director of pediatric intensive care.
"He convinced me," says Levin, "that the change to another environment—both geographical and to a different kind of hospital/ university/medical school environment— but still doing the same kind of thing I was doing, just on a much smaller basis, would accomplish the things I wanted to and would be less stressful than becoming a director of a pediatric hospital or trying to work with industry."
Levin arrived at Dartmouth in 1996 and helped to design and build a new, state-ofthe art, spacious six-bed PICU that opened at the Children's Hospital at Dartmouth in 1999. Plans are now underway to open four more beds. Staff as well as patient and family focus groups had a hand in the design of the unit; suggestions included putting daybeds and rocking chairs in each room and building a dormitory-style sleep area nearby, so parents could easily stay overnight with their sick children.
Currently, he is introducing to the PICU a new staff role—a pediatric advanced nurse practitioner—a model that he says is "reasonably new around the country." He has also helped to reorganize the DHMC transport service and to establish a mobile intensive care unit.
"Some people have looked at it sort of funny—my coming from this huge program in Dallas," says Levin. He points to a group photo on his office wall. "That was my section in Dallas . . . it was as big as the department of pediatrics here. Most of the other people who ran very big programs like that don't do intensive care medicine any more."
But coming to Dartmouth has allowed Levin to continue practicing pediatric critical care medicine—and spend time with his three college-aged children, as well as fly-fish, ski, and bike. "It's a young man's game—intensive care," Levin laughs. "But I'm almost 58, been in medicine for 31 years. I've been in intensive care full-time on a faculty level for 26 years and I'm still doing it." And, clearly, still loving it.
Laura Carter is the associate editor of Dartmouth Medicine magazine.
