Vital Signs
DHMC is acquiring a growing family of simulated patients
"What you see are hours of boredom punctuated by moments of terror," says Marc Bertrand, M.D., the director of DHMC's anesthesiology residency program. He's explaining to a group of residents the management of rare moments of crisis—such as cardiac arrest and major trauma— that they'll encounter in emergency rooms and operating suites. Luckily, these trainees will first encounter such emergencies not in real patients but in sophisticated mannequins.
Bertrand's course on crisis management uses two high-tech simulated patients: an adult and a child. Each is hooked up to a computer console with a myriad of wires. An engineer at the console can control the simulator's cardiovascular, pulmonary, and neurological systems and replicate a variety of scenarios: from aortic clamping to emergency hypertension to snake bite.
|
|
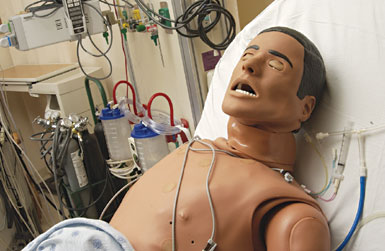
This patient doesn't appear to be doing
well. But not to worry—it's a plastic
simulator, one of several at DHMC. |
In Bertrand's day-long crisismanagement course, residents work through several advanced cardiac life support (ACLS) scenarios. "They can listen for breath sounds, feel pulses, place IVs, and check the pupils," says Bertrand, noting that the mannequins' pupils can be made to dilate or constrict. Trainees also learn how to place a breathing tube while the engineer manipulates the controls to, say, block the airway or simulate a dropped lung. The mannequins can even be hooked up to monitors so residents can check their blood pressure, pulse, heart action, and respiratory gasses.
Chaos: Each simulator also has a speaker in its head, so Bertrand or an assistant can "talk" for the "patient"—answering questions or relating symptoms in an eerily lifelike way. "You really are able to reproduce some of the chaos and hectic nature of a real crisis," says Bertrand.
He and his colleagues are especially interested in teaching anesthesiology residents the behavioral aspects of managing crises. This involves defining a team leader and establishing good team communication. In the OR, for example, the anesthesiologist generally takes the role of team leader, while surgeons focus on specific procedures. This "can be the toughest thing to get the resident staff comfortable with," says Bertrand. "You want to do the procedural aspects yourself."
Other departments besides anesthesiology use the mannequins, too. The child simulator is used to teach pediatric sedation and pediatric airway management. And fourth-year medical students use the adult simulator for ACLS training.
Obstetrics has its own specialized simulator for teaching emergency C-section procedures. This mannequin has a birth canal with a motor that actually delivers a baby. These training sessions involve nurses, physicians, and residents from anesthesiology, obstetrics, and neonatology. "Compared to other institutions," says Bertrand, "this is a far more rich sort of approach to team training . . . more realistic, more reflective of what we encounter in our practice."
Nursing, which is starting a nurse residency program soon, is about to acquire two new simulators. Nurse residents will be trained in high-risk but low-frequency respiratory and cardiac emergencies. They'll learn, for example, how to provide oxygen therapy, start an IV, administer medication, and obtain test results if a simulator complains of chest pain. "It gives you the opportunity to create simulation experiences that new nurses might take years to encounter," says Nancy Formella, M.S., R.N., senior nurse executive at DHMC. Funding for the simulators has come from a variety of sources, including gifts.
Tools: "Everyone is involved in building these resources," explains George Blike, M.D., director of patient safety. "These tools are beneficial—participants learn faster, learn better, and retain it longer."
Matthew C. Wiencke
